What Actually Happens Inside the OT During a C-Section?

Dr Mannan Gupta
Medically Reviewed by Dr. Mannan Gupta On May 12, 2026
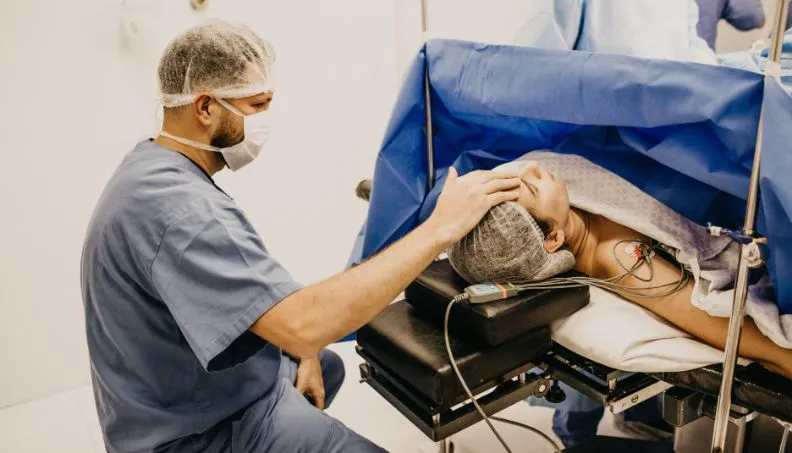
A caesarean section is a major abdominal surgery that takes approximately 45 to 60 minutes from the first incision to the moment you hold your baby — and every step inside the operating theatre is carefully choreographed to keep both you and your newborn safe.
Most patients walk into the OT anxious simply because no one has ever explained what actually happens inside. That changes today.
At Dr. Mannan IVF Centre, New Delhi, Dr. Mannan Gupta, High-Risk Pregnancy and IVF Specialist, believes that an informed patient is a calmer, more confident patient.
As one of the trusted C-section delivery hospitals in New Delhi, we walk every mother through what to expect — before, during, and after surgery.
Key Takeaways
- A C-section involves multiple coordinated layers of incision, delivery, and closure — not just “cutting and pulling”
- You are awake during most C-sections; spinal or epidural anaesthesia is standard, not general anaesthesia
- The baby is typically delivered within the first 10–15 minutes; the remaining time is surgical closure
- A sterile operating theatre team of 6–8 specialists works in sync throughout the procedure
- Skin-to-skin contact with your baby is possible even in the OT in many cases
- Knowing what to expect significantly reduces pre-surgical anxiety
Who Is in the OT and What Is Their Role?
Walking into an operating theatre can feel overwhelming — bright lights, unfamiliar equipment, masked faces. Understanding who each person is immediately makes it less intimidating.
A standard C-section team includes:
- Obstetrician — performs the surgery
- Assistant surgeon — supports retraction and closure
- Anaesthesiologist — administers and monitors anaesthesia throughout
- Scrub nurse — handles sterile instruments directly
- Circulating nurse — manages the OT environment and documentation
- Neonatologist or paediatrician — receives and assesses the newborn immediately after delivery
Every role is essential. The coordination between these professionals is what makes caesarean delivery one of the safest surgical procedures in modern obstetrics when performed in a properly equipped facility.
What Happens Before the Surgery Begins?
Preparation inside the OT begins well before the first incision. This phase typically takes 15–20 minutes and is just as critical as the surgery itself.
Positioning and anaesthesia come first. You are helped onto the operating table and positioned with a slight left lateral tilt — this prevents the uterus from compressing the major blood vessels that supply your lower body.
A spinal block (most common) or epidural is then administered by the anaesthesiologist. You will feel pressure but no pain from the chest downward within minutes. A urinary catheter is placed after anaesthesia takes effect.
A sterile drape is positioned between your chest and the surgical site — you will not see the incision, but your partner or support person (where permitted) may be seated near your head.
Your blood pressure, oxygen levels, and heart rate are monitored continuously on a screen throughout.

Dr Mannan IVF Centre
Experience world-class fertility care with Dr. Mannan Gupta at the Best IVF Centre in Delhi
How Is the Incision Made and What Layers Are Cut?
This is the part most patients are most curious — and most misinformed — about.
A planned C-section delivery almost always uses a Pfannenstiel incision — a low, horizontal cut made just above the pubic hairline, roughly 10–15 cm long. This is commonly called a “bikini cut” and heals with minimal visible scarring.
The surgeon then passes through multiple distinct layers:
- Skin — the outermost layer
- Subcutaneous fat — separated bluntly, not cut
- Fascia (Rectus sheath) — a tough connective tissue layer opened carefully
- Rectus abdominis muscles — gently separated, not cut
- Peritoneum — the inner lining of the abdominal cavity, opened to access the uterus
- Uterus (lower uterine segment) — the final and most critical incision
Each layer is handled with precision. The goal is minimal tissue trauma, reduced blood loss, and faster healing.
How Is the Baby Actually Delivered?
Once the uterus is opened, delivery happens quickly — usually within 2 to 5 minutes of the uterine incision.
The surgeon reaches in and guides the baby’s head (or presenting part) out through the incision.
Gentle fundal pressure — applied by the assistant on your upper abdomen — helps ease the baby out. You will feel significant pushing and pulling pressure at this moment. This is normal and expected.
The umbilical cord is clamped and cut. The baby is handed immediately to the neonatologist, who assesses breathing, muscle tone, and heart rate using the Apgar score — a quick 10-point evaluation done at 1 and 5 minutes after birth.
If the baby is stable, skin-to-skin contact in the OT is increasingly offered at progressive maternity hospitals for C-section in New Delhi and is something we actively facilitate at our centre where clinically safe to do so.
Preparing for a C-section and want to know exactly what to expect? Speak with Dr. Mannan Gupta directly — get honest, expert answers before your delivery date. Dr. Mannan Gupta at Dr. Mannan IVF Centre, New Delhi.
What Happens After the Baby Is Delivered?
The remaining 30–40 minutes of the surgery — after your baby is born — focus entirely on careful, layered closure.
The placenta is delivered first, either spontaneously or with gentle traction. The uterus is inspected, and the uterine incision is closed in one or two layers using absorbable sutures.
Each abdominal layer is then closed in reverse order — peritoneum, fascia, subcutaneous tissue, and finally skin.
Skin closure is done using subcuticular sutures (hidden under the skin) or surgical staples, depending on the surgeon’s approach and patient factors.
Throughout this phase, the anaesthesiologist continues monitoring your vitals and managing any pain or discomfort. Blood loss is carefully measured.
Most cesarean delivery procedures involve a blood loss of 500–1000 ml, which is within expected and manageable limits for a prepared surgical team.
What Do You Feel and Experience During the Surgery?
You are awake. You are aware. And that can be unsettling without preparation.
You will feel pressure, pulling, and movement — but not pain. Some women describe a sensation like “someone rummaging through a bag near my stomach.” That is accurate, and it is normal.
You may feel nauseous briefly, particularly when the uterus is exteriorised for inspection in some surgical techniques. The anaesthesiologist can manage this immediately with medication.
Shivering is common after spinal anaesthesia — caused by the medication’s effect on body temperature regulation, not cold. Warm blankets and reassurance are standard responses.
Emotionally, hearing your baby cry for the first time from behind that drape is a moment patients describe as surreal, overwhelming, and unforgettable — regardless of how the delivery was planned.
What Immediately Follows in the Recovery Room?
After surgery, you are moved to a post-anaesthesia care unit (PACU) or recovery room for 1–2 hours before transfer to your ward.
During this time, the care team monitors your blood pressure, uterine firmness, bleeding, and sensation returning to your legs. Pain medication is administered proactively so you are comfortable before the spinal anaesthesia wears off completely.
Your baby, if stable, is brought to you here for initial feeding and bonding. Early breastfeeding — ideally within the first hour — is actively encouraged as it supports uterine contraction and milk production.
If you are considering your options for future deliveries, you may want to learn more about Is VBAC Safer Than Having a Second C-Section? to understand the long-term surgical considerations.
Conclusion
A C-section is not something that simply “happens to you.” It is a precisely coordinated surgical procedure involving a full team dedicated to one outcome — your safety and your baby’s wellbeing.
At Dr. Mannan IVF Centre, we believe demystifying the operating theatre is part of good obstetric care. When you understand what is happening at each step, fear gives way to trust — and trust makes the entire experience better.
If you are scheduled for a C-section delivery or are still deciding on your birth plan, come speak with us. Knowledge is the best preparation you can have.
Frequently Asked Questions
1. Will I be put to sleep for a C-section?
In most cases, no. Spinal or epidural anaesthesia keeps you awake but completely pain-free from the chest down. General anaesthesia is reserved for specific emergencies where regional anaesthesia is not safe or fast enough.
2. Can my husband or partner come into the OT with me?
Many hospitals allow one support person in the OT during a planned C-section. This depends on hospital policy and whether the situation is elective or emergency. Always confirm this in advance with your care team.
3. Why do some women vomit during a C-section?
Nausea and vomiting during C-section are common and related to blood pressure drops from spinal anaesthesia or uterine manipulation. Anaesthesiologists anticipate this and have medications ready to manage it quickly.
4. Is it true the baby's head can get stuck during a C-section?
Occasionally, particularly in emergency cases where the baby is deeply engaged in the pelvis, delivery through the uterine incision can be technically challenging. Surgeons are trained for this and use specific manoeuvres — including the “push” technique from below — to safely deliver the baby.
5. Does a C-section affect bonding with the baby?
Research does not support the idea that C-section delivery inherently impairs bonding. Skin-to-skin contact, early breastfeeding, and presence during the newborn’s first assessments all support attachment — and these are all possible after caesarean birth with appropriate support.
